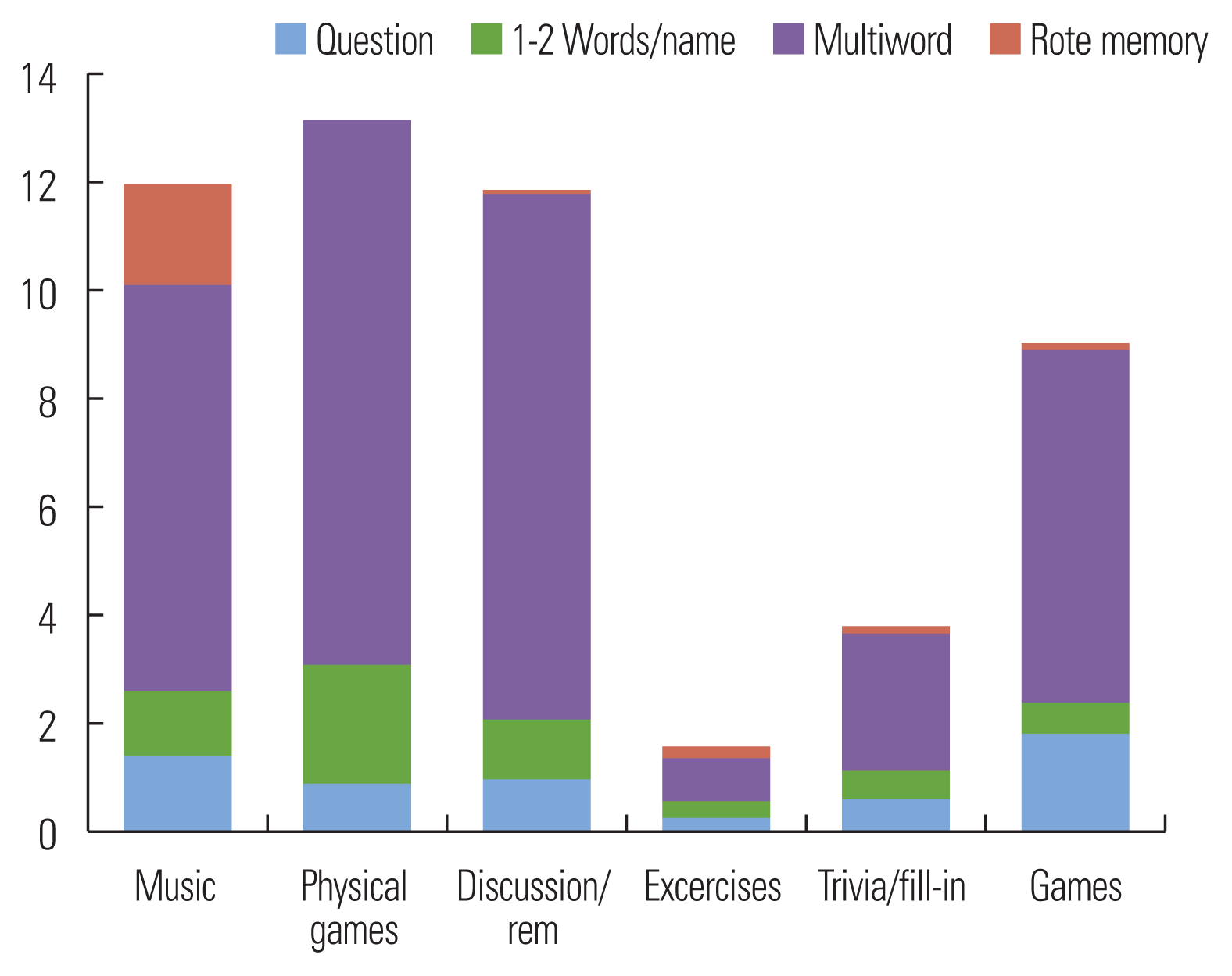Clune, Hewitt, Archer, and Lee: Communicative Behaviors Elicited by Leisure Activities in Memory Care Units
Abstract
Purpose
In this exploratory study, patterns of vocal communication elicited by different activities facilitated in a unit were examined. Research questions included: Do different activity types elicit more or less vocal communication? How do participants vary in terms of rate, type, and activity contexts for their vocal communication attempts? What patterns of interaction among residents and staff were observable during group activities?
Methods
Data were collected using a live data collection tool, divided by vocalization type, and qualitative notes were taken for each activity and participant. Four participants with varying stages of dementia were included in analysis. Coding reliability was conducted on 43% of samples, with utterance function codes at 99% and vocalization types at 75% agreement.
Results
Overall, the activity that elicited the most vocalizations for 3 participants was physical games, while the two activities that were consistently in the bottom range of total number of vocalizations were trivia/fill-in and exercises. Participants with substantial impairments in cognition appear to initiate communication more often during physically-based activities with clear turn-taking roles.
Conclusions
Results suggested that diversity of ability among residents must be skillfully handled by staff to promote residents’ equal participation. Suggestions for improving activity facilitation based on activity types and facilitation strategies are offered.
Keywords: Dementia; Alzheimer’s disease; Communication; Vocalizations; Leisure activities
INTRODUCTION
Communication difficulties that result in social isolation and lower quality of life are well known to occur in individuals with dementia. Kempler and Goral note that, in most cases, dementia impacts multiple areas of cognitive function, leading to impairment in language functioning secondary to deficits in memory, attention, and executive functioning, all of which in turn are linked to communication impairments such as anomia and sentence processing problems [ 1]. Families, friends, spouses and caregivers report the impact that reduced communication has on personal relationships. In their review on dementia’s impact on communication, Byrne and Orange [ 2] stated that communication is one of the first losses reported in dementia, with 24% of spouses listing breakdown of communication abilities as the most difficult part of the disease, ranking its effects above memory loss, aggression, and uncooperative behavior. Caregivers also report that the loss of communication and relationship is stressful and painful (see Bayles & Tomoeda, 1991, for a review) [ 3, 4] (see Bayles & Tomoeda, 1991, for a review). Communication plays a crucial role in creating and maintaining relationships, which in turn have a positive effect on mental and functional health [ 4, 5]. Communication is very important for PWDs’ maintenance and creation of relationships. Their ability to create new memories and common ground with others is lost as the disease progresses, thus requiring construction of relationships in the moment of interaction [ 6, 7], thus requiring construction of relationships in the moment of interaction. Individuals with disabilities residing within residential facilities frequently experience social isolation. Residents of nursing
homes have been found to spend as much as 65% of their time doing nothing, or participating in passive activities such as watching a music performance [ 8]. One suggested cause of this isolation is the infrequency of social communication, because PWDs have a decreasing amount of social engagement with their caregivers. This isolation makes activities and visits a crucial opportunity for communication stimulation to combat an ongoing problem experienced in assisted living facilities [ 3]. Despite its importance, there has been little investigation of what types of supports and activities best promote communicative success and social engagement in persons with dementia. Attempts to remediate the difficulties experienced by PWD’s include distraction elimination, simplifying sentences, and yes-no questions [ 9, 10]. Small & Perry [ 10] explored the role of question types in responses of persons with dementia, finding that caretakers used yes-no and open-ended questions equally; however, episodic-memory-based questions (questions regarding specific events) were used nearly twice as frequently as semantic-memory-based questions (questions regarding general knowledge). Although yes-no questions were generally more successful, open-ended questions were successful when they were tapping semantic, as opposed to episodic, memory [ 9, 10]. There is little information about which specific strategies are most successful and the literature offers at best preliminary guidance on techniques that lessen communication breakdowns for PWDs. The importance of promoting opportunities for social interaction and communication is widely recognized, even if information on what discourse structures and types of activities are best for fostering successful linguistic communication in PWD’s is lacking. Participation in stimulating activities is generally beneficial to mental health and cognitive function [ 4, 11] as is social engagement with peers [ 4]. In addition, activities help residents maintain the ability to perform daily living activities, [ 11] and engaging in activities is associated with fewer anxious behaviors [ 12], while a lack of activity has been linked to more behavioral problems, isolation, lower cognitive function and reduced quality of life [ 4]. Activities in which PWDs are interacting with others in a supportive environment (i.e., group activities) provide opportunities for practicing appropriate behavior, promoting physical function, interpersonal management strategies and communication. Well-designed activities therefore have a positive influence on social-affective functioning [ 4, 12]. Prior research on what constitutes well-designed activities for individuals with dementia has provided some initial guidance for best practices. Activities using tangible stimuli (e.g., toys or dolls) appear to elicit more meaning-enriched statements (i.e., statements containing specific information the PWD wishes to communicate) [ 11, 13]. Other research suggests that social stimuli increase communication more than nonsocial [ 13, 14]. Social stimuli inherently promote communication, as they can prompt recall of familiar social experiences, such as pets, friends, or children. While structured activities have their place, the importance of social engagement suggests an important role for conversation as an alternative to more structured activities. Although challenging, the naturalness of conversation is beneficial, appealing to participants who do not enjoy structured activities [ 6]. Natural conversation can create opportunities for PWDs to support each other in social situations [ 7]. In addition, conversation with peers creates safe spaces for PWDs to express habitual memories (i.e., memories that they lived often), thus constructing identities for themselves [ 6]. The expression of these memories is crucial to role development because they tell the PWD’s story to others that may not have known much about them. They also create a shared experience (the story) on which the relationship between two individuals without much memory can be based. Reminiscence therapy is an activity involving conversation. In these interactions, the topic of the conversation is controlled to focus on pictures, personal items, media or past activities [ 15]. Reminiscence therapy is linked to positive mood, behavior, and cognition outcomes, but a structured and well-designed approach is necessary for success [ 15, 16]. Despite general agreement that group activities are beneficial for persons with dementia, the literature providing guidance to clinicians and other professionals charged with developing activities is slim. Several studies suggest that speech-language pathologists as professionals should facilitate group activities for persons with cognitive-communication disorders secondary to dementia, or at risk for such disorders, to foster communicative exchanges and help preserve abilities [ 2, 17- 19]. By conducting a preliminary examination of communication during everyday group activities in a memory care unit, the present work undertook to begin to address this gap in the literature. We explored the impact differences among activities have on communication of PWDs as they interacted with staff and visitors during their regularly scheduled leisure programming, exploring types of participation and patterns of participation across different activity types. The following research questions were posed:
Do different activity types elicit more or less vocal communication? How do participants vary in terms of rate, type, and activity contexts for their vocal communication attempts? What patterns of interaction among residents and staff were observable during group activities?
To answer questions 1 and 2, PWDs residing in a residential facility participating in their regular activities were observed, and data were taken on vocal communication elicited by different types of daily leisure activities for each participant. (Non-verbal communication was not studied, owing to limitations in feasibility for coding non-verbal communications in a live, on-line procedure.) The third research question was addressed by compiling contextual notes. Descriptive statistics are reported, accompanied by a qualitative narrative analysis of patterns of interaction.
METHODS
Participants
This study took place in a memory care unit in a small town in the Midwestern United States. It was approved by the Institutional Review Board of Bowling Green State University [BGSU-IRB# 902580-10]. Inclusion criteria for the study were that the participants have a formal diagnosis of dementia, and regularly took part in activities in the facility. Four participants exhibiting various types of dementia and language functioning met these criteria and took part in the study. Participants’ legal powers of attorney provided consent and a simplified verbal assent was read to each participant.
P1was an 89-year-old male diagnosed with Alzheimer’s dementia, who entered the facility with his wife (P2) approximately 1 year before this study. P2 was an 85-year-old female, diagnosed with senile dementia, in addition to various previous mental health issues, and an embolism. P4 was a 77-year-old female with general dementia, who entered the facility 3 months prior; she also was previously diagnosed with depression, and had undergone noncancerous brain surgery. P5 was an 83-year-old male diagnosed with Alzheimer’s disease, who had been in the facility for approximately one year. All diagnoses are given quoting the wording in the medical records. (Note: one additional participant, P3, was initially recruited, but was excluded owing to lack of formal diagnosis and low participation.)
Collection procedure
A paper tally sheet was used for data collection (see Appendix B). Data collection was done in pairs by the primary investigator and one of three research assistants, a graduate student in speech-language pathology and two undergraduate students in communication sciences and disorders. Each of the assistants attended different collection sessions. Researchers placed tallies in the appropriate section for the observed participant and vocalization type as the activity session progressed. The principle investigator also took pertinent notes on the context of the activity, participants’ engagement, patterns of communication, or interactions. Each data collector coded the behavior of 3 participants (maximum) during a session, so at least 1 participant was coded by two researchers, to check for inter-rater reliability.
Data collection tools
The tool used in this study was based on Halliday and Mathiessen [ 20] functional approach to language analysis by considering the purpose behind “messages”. Halliday [ 20] suggests that in exchanges, the speakers take on different roles that can be labeled as either “giving” or “demanding” of either “goods-&-services” or “information”. These four basic identifiers can be combined to create the four basic types of messages, representing basic communicative functions: offer, demand, statement, or question. The coding sheet for our study was based on this approach; because the Halliday and Mathiessen [ 20] categories focus on purposes of communication, using a simple matrix, it was well-suited to our need for a tool that could capture significant aspects of interaction while sufficiently simple in that it was workable for live data collection. The statement category was broken into two sections: 1–2 word utterances or names, and multiword utterances. This separation was to show variance in the amount of information provided in the statement. Based on a trial period using the coding system, a few additional categories were added: exclamations (showing surprise or concern); rote memory (overlearned language, e.g. lyrics, nursery rhymes, common sayings); nonword vocalizations; and unintelligible utterances. In addition to the coding of vocal output, engagement scores were coded, from 1 (none) to 7 (maximum), and affect (negative, flat, or positive). Engagement was defined as whether the participant appeared interested in the activity, and was participating actively, while affect was defined as the participant’s emotional appearance during the activity, using the three categories upset, neutral, or happy. We arrived at the final form of the data coding sheet after piloting and feedback from the first reliability coder. The coding manual can be seen in Appendix A.
Analysis
To analyze the collected data, the activities were first grouped based on type of participation, to address research question 1. Data collected during individual activities, such as newspapers, puzzles, or manicures were not included because the communicative context was not comparable to that of the usual group activity. In addition, only activities with at least 3 sessions observed were used, to provide sufficient exemplars to support analysis, and avoid the possibility that differences were based on how the participant was functioning on one specific day rather than activity type. The exclusion of activities with less than 3 sessions of code led to the exclusion of artistic activities for all participants, and of games for participants 1 and 2.
Activity types:
Trivia/fill-in: activities that utilized questions with multiple choice answers, naming of items that fit certain descriptors, or fill-in the blank phrases or lyrics Exercises: morning chair exercises led by a facilitator Physical Games: games played that required more physical engagement Music: Activities that utilize music as the focus of the activity Discussion/Reminiscence: Activities in which the main form of engagement is discussion, usually about a selected topic that is sometimes reminiscence based Games: Activities that included cards or games Artistic: Activities that required participants to use creative skills
Quantitative data
To ensure consistency, if there were two sets of data for one session (the principal investigator’s and the reliability coder’s), only the principal investigator’s code was used. This decision was made because the principal investigator had established reliability with all coders. The total minutes for each activity were added, then divided by 5, to establish the frequency per 5 minutes of the activity, the total number of each vocalization type was summed, and divided by the rate obtained above. These resulted in a rate of type of vocalization per 5 minutes, for each activity. These calculations were made for each participant and activity type.
Reliability
To calculate reliability, the number of agreed upon communicative acts was divided by the sum of agreed and disagreed upon acts for each type of vocalization; 64 of the 148 (43.24%) total sets of data were coded for reliability, with the average score for individual vocalization types at 75%, and total utterances at 99.3% reliability. At least one participant per coding session out of the total data sets available was scored for reliability.
Although reliability overall was high, three categories received lower reliability scores: Offers 13% (3/22), Unintelligible 49% (42/86), and Exclamation 67% (52/78). Although these weaknesses are concerning, the most significant categories for this project are Question (98.7%), 1–2 Word (99.4%), Multi-Word (98.0%), and Rote Memory (97.7%). These categories had the most overall tallies in the study, and as noted by the reliability scores, were the most consistent.
RESULTS
Overall, the activity that elicited the most vocalizations for P1, P2, and P5 was physical games, while the two activities that were consistently in the bottom range of total number of vocalizations for these three was trivia/fill-in and exercises. Conversely, P4 produced the most total vocalizations during discussion/reminiscence, and the least total vocalizations during physical games. Discussion/reminiscence activities elicited the least number of vocalizations for P2, and a mid-range number of vocalizations for P1 and P5 as compared to the number of vocalizations elicited by other activities.
Participant 1 (P1)
P1 displayed the most total vocalizations during physical games, a majority of which were 1–2 words/names or multiword statements. However, P1 asked the most questions during discussion/reminiscence, which, along with exercises, elicited a mid-range number of total vocalizations as compared to other activities. Finally, music and trivia/fill-in elicited the least total utterances from P1 compared to other activities. See Table 1 and Figure 1 for details.
Participant 2 (P2)
P2 produced the most vocalizations during physical games compared to other activities, most of which were multi-word utterances. However, P2 produced the most questions and 1–2 words/phrases during musical activities, which elicited the second most total utterances of the activities. Finally, trivia/fill-in activities and discussion/reminiscence activities elicited the least total vocalizations compared to other activities. See Table 2 and Figure 2 for details.
Participant 4 (P4)
P4 produced the most vocalizations during discussion/reminiscence activities compared to other activities, followed closely by trivia/fill-in activities. Music and games elicited the lowest total number of utterances compared to other activities. P4 consistently used more total vocalizations during discussion/reminiscence—her use of multiword phrases was also more frequent during these activities. See Table 3 and Figure 3 for details.
Participant 5 (P5)
P5 displayed the most vocalizations during physical games compared to other activities, closely followed by musical activities and discussion/reminiscence activities. Finally, trivia/fill-in and exercises elicited the fewest total utterances for P5 compared to other activities. See Table 4 and Figure 4 for details.
General observations
In addition to numerical data, we also took observational notes in order to do a qualitative analysis to address research question 3: What patterns of interaction among residents and staff were observable during group activities? A synthesis of notes revealed patterns and contextual information about interactions.
Physical games
The most common game played was noodle ball, which is played using a portion of a pool foam floating aid (known as a “noodle” because of its shape) to bat around a balloon to prevent it from hitting the floor. Based on the amount of enthusiasm and participation displayed by participants, this game was a clear favorite for a majority of the residents.
Exercises
The participants tended to match the amount of enthusiasm displayed by facilitators during this activity, although it usually peaked during the “dancing song”, which was an upbeat, popular current song. One interesting interaction occurred during a morning exercise session lead by the intern. P2 tapped her foot to the music between different exercises. This action was then used as a new addition to the exercise routine. When P2 noticed that her action was taken as a suggestion, she became visibly more enthusiastic and verbal in both exercises and subsequent activities.
Trivia/fill-in
Trivia/fill-in activities usually elicited little enthusiasm; 13 field notes reported that all but P4 were asleep, and 4 notes that those who did answer appeared unengaged based on their low affect. This activity also tended to result in participants taking part in alternative activities (e.g., singing, eating), or simply by disengaging, ignoring the activity altogether. Participants regularly remembered answers but could not provide their meanings, and had trouble with the confrontation naming required by the fill in the blanks nature of the questions.
During this activity, a pattern of engagement by facilitators with less experience (e.g., new employees and new interns) emerged. These inexperienced facilitators overwhelmingly chose to engage P4 and others (not participating in the study) exhibiting higher cognitive and communicative abilities over others in the group who were less linguistically able. Facilitators also returned to P4 for answers more often and waited longer for her to respond. When facilitators did ask other participants directly, they rarely returned focus to a participant whose turn was interrupted. Another difference noted during this activity was that more experienced facilitators tended to enunciate better, and use more concise language with visualizable examples.
Discussion/Reminiscence
Discussion and reminiscence were based on photos, videos, or reading from a newspaper, book, or the facility’s activity software. Energy levels during this activity varied greatly. It was noted 5 times that the interaction was dominated by P4 and the facilitator, aligning with notes that P4 tended to be asked more direct questions than P1, P2, and P5.
Although the uneven pattern of conversation noted in the previous paragraph was common, the “M&M Game” appeared to be an exception. This game used the different colors of the M&Ms as stimuli representing different topics, including the local university (orange), pets (red), jobs (blue), kids (yellow), hometown (brown), and cars (green). The facilitator would choose a color to speak about, and ask each participant if they had the color. If they had the color, they were asked to talk about that subject, and scaffolding was provided if they struggled to provide spontaneous responses, Because of the imposed turn structure, a more equal distribution of turns was observed. One example of this was when P4 attempted to interrupt P1’s turn and was curbed by facilitators to allow P1 to finish his turn.
Collectors observed a few concerns during this activity type for all participants. Confronting questions, which are often challenging for this population because they ask the PWD to directly provide exact information on a specific topic, were a point of struggle for most participants. These questions sometimes caused participants to be unable to discuss information that they had casually discussed previously. When facilitators re-formed questions into yes-no format, more success was observed, along with further discussion based on the scaffold. Finally, it was also noted that activities relying solely on verbal input as a stimulus (such as reading aloud) were associated with lower engagement.
Music
Musical activities usually included music videos or karaoke from the facility’s computer program, or P4 playing piano for the group. In the use of the computer program, the facilitator would either sing along with the residents, or leave the room. When participants were left alone, it was common for all participants to fall asleep, or become distracted. During P4’s performance, more relaxed engagement by way of conversation in dyads was observed.
Games
The games section refers to either a dice game entitled “Over the Mountain”, or a card game entitled “Stick or Switch”. The dice game was only played once and was not well-received, with P4 and P5 becoming agitated by the lack of goal or purpose. Conversely, cards resulted in higher energy, and, in P5’s case, increased interaction.
Participants and Facilitators
Participants 1 and 2 interacted with one another most; however, they both occasionally attempted to join in group conversation. These attempts were unsuccessful because of inability to take the floor without support from a facilitator, and cooperation from the dominating resident. P5 did not have many difficulties establishing his turn, but he was interrupted regularly by the more dominant participant after which he did not usually regain the floor to finish his response. Although large group conversation had varied results, dyadic conversations during piano music, and conversations using turn-structure seemed significantly more successful in terms of communicative opportunities for slower-to-speak participants. P4 displayed very different patterns of communication. One notable observation from her interactions was the use of clarifying questions. P4 was also noted to interrupt repeatedly in 12 different sessions.
Facilitators’ interactions with P4 were also different than their interactions with the other participants. Because of the appearance of higher ability level in P4, facilitators often relied on her during activities. Examples of this include her opinions being solicited exclusively, and the higher number of direct requests and returns to P4 received from staff. Finally, she was sometimes allowed to talk over other contributors.
DISCUSSION
Communication and activities
Music
Previous research has found that music can increase engagement and minimize agitated behaviors [ 16], especially when the songs are matched to listener preferences [ 21]. However, in this study, musical activities showed a wide range of results. When activities relied on a computer program displayed on a screen, overall engagement was relatively low, potentially because of lack of social stimuli [ 13, 14], and the low visibility of karaoke words. Piano music elicited a more relaxed type of interaction in which no topic was specified and large group interaction was not expected. The non-directed nature of the activity may have encouraged two participants to interact more in dyads, a type of conversation that PWDs tend to have fewer difficulties with [ 6]; perhaps because of the simplification of turn-taking. According to Eggins and Slade [ 22], a large part of turn-taking is the current speaker’s role in selecting the next speaker with verbal or physical cues. However, in the absence of a selection, participants are able to self-select. Self-selection during casual conversation can lead to confusion, lulls in conversation, and, in this unique situation, often leads to conversation domination by a more communicatively able participant. Turn-taking was simplified by only having a speaking partner as opposed to a whole group to share the floor with. Conversation in larger groups (e.g. discussion/reminiscence) was more challenging for the less linguistically-able participants. During large group activities, these two participants made many attempts to enter the larger conversation, but often were not able to establish themselves and take regular turns. Although dyadic conversation gives opportunities for participation, as Goodwin [ 23] points out, they can alienate other speakers, turning them into audience members. While small spans of time as audience members may be harmless, becoming an audience too often can cause participants to disengage, as exemplified by activities which had lower numbers of communicative acts for these slower to speak participants. One conclusion from this finding is that facilitators need to consciously provide opportunities for equal engagement when promoting conversation-based activities.
Physical games
Physical games elicited the most total vocalizations for 3 of 4 participants. Very little literature was available about physical games used with PWDs, but one reason for these results could have been the presence of tangible stimuli, which are thought to produce more meaning-filled statements ,that is, utterances with more semantic detail that are not simple responses [ 11, 13]. In addition, the structure of games such as noodle ball requires both communicative interaction with others as well as physical participation. It may be that participants preferred physical engagement, or possibly the physical activity itself promoted a higher level of awareness and ability to focus, which in turn fostered more attempts at communication. All of these factors suggest turn-taking games with physical activity have the potential to be good contexts for communicative engagement among persons with dementia. Many games embed a turn-taking structure, naturally drawing attention to the person whose turn it is and giving them the floor. This structure encourages more shared interaction among participants with varying levels of ability. The framework typically includes the group observing the shared object of the conversation, followed by talking about it, or in some types of activities using gesture, posture, or completion of tasks, to continue the activity while the facilitator provides scaffolding. Furthermore, organization of bodies within the space during structured games typically allows for shared attention and actions [ 23]. In noodle ball, for example, the participants form a half-circle facing the facilitator, who continuously tracks and distributes turns hitting the balloon. When a participant bats the balloon to another participant, they are selecting the next turn based on the shared object of interest. This structure contrasts with the self-selection occurring during lower-structured activities, which favor the more linguistically able, and can cause them to dominate the discussion. However, it resembles the lower-structured activities in that there is room on the floor for spontaneous conversation, as well as a need to relate to others playing. This small amount of extra flexibility can encourage more conversation than overly structured activities, such as trivia, where a specific communication is expected.
Discussion/reminiscence
Discussion/reminiscence activities were the least successful in eliciting vocal contributions from 3 of the 4 participants. One participant produced the most vocalizations during this activity. Nijhof et al. [ 15] reported reminiscence as effective in eliciting communication. Cabrera [ 16] suggested that reminiscence and discussion for groups of PWDs are most successful when they are structured and well-designed. Structure may be important in maximizing participants’ opportunity for engagement; similar results have been reported in aphasia group therapy [ 24]. The uneven linguistic and cognitive abilities in the group we observed may have led to the uneven participation levels; more care in structuring the linguistic framework and turn structure of these activities would appear to be needed if various levels of ability are to be supported. For the participant who was highly vocal during these activities, her relative lack of need for prompting was a likely factor. Others needing more structure could not engage. One may further speculate that pragmatic challenges of a participant who can take a turn but does not know how to yield a turn will depress others’ participation further. This participant also did not appear to be aware of topic maintenance, or self-regulation in turn-taking or interruptions.Despite her pragmatic challenges, facilitators did not redirect her, perhaps because of the appearance of higher conversational skill leading facilitators to rely on her. Because of the unique communication limitations experienced by these participants, they are in need of special support to continue the conversation. If facilitators are not prepared to take on strong initiating roles by using more opening statements, they will create a framework that relies more heavily on the few that produce rejoining moves [ 22]. Although the results for discussion/reminiscence found in this study were mixed, previous literature suggests that conversational activities have many unique benefits for PWDs in terms of both individual well-being and social interaction, helping with formation of relationships and identities [ 7]. There also is evidence that conversation appeals to participants who typically are not interested in activities [ 6]. Therefore, further investigation for successfully facilitating discussion is warranted, and the need for caregiver training in effective management of groups of disparate ability is also suggested.
Exercises
Exercises elicited few vocalizations overall. It could be hypothesized that exercise requires more attention and concentration, with no defined turns because the activity was continuous. This focused and continuous demand on concentration means that, to join conversation, participants must split their attention between doing the exercises and putting together verbal input. According to Mahendra [ 11], dementia is often accompanied by the decline of ability to focus attention, and therefore, difficulty focusing on multiple characteristics of a stimulus. While Mahendra [ 11] does not specifically refer to multi-tasking, it could be hypothesized that the idea generalizes to this situation.
Trivia/fill-in
Trivia/fill-in activities were the lowest or second lowest communicative activity for 3 of the 4 participants, showing once again that activities can result in individual differences. One participant produced the second most vocalizations during this activity. This relative success might be attributable to her more spontaneous and frequent responses to prompts than her peers, allowing her to answer before other residents could have fully processed the question. Similar to her engagement in the reminiscence activities, this participant received more direct prompts from facilitators, and she used unique strategies to regain or retain the floor, the most prominent of which was asking questions to either extend her turn or interrupt others.
A plausible reason for the lack of communication by other participants could be the format of the questions used, which required highly specific answers, often based on events in the past. Overall, yes-no questions are the most successful for PWD’s, while open-ended questions are best used only with information from semantic as opposed to episodic memory [ 9, 10]. Therefore, trivia questions about semantic rather than episodic information in either format could be more successful.
Games
Games have a naturally occurring turn-taking structure that appeared to facilitate participation for the less linguistically and cognitively able participants. There was less dominance by the more linguistically able participant. The natural occurrence of turns in such activities as card games provide a clear framework that is not easily violated and allows for more equal participation.
Implications
Activities
This study suggests that activities may be more successful when conducted by a live facilitator, who serves as a social stimulus; computer-based prompts were notably poorly received by the participants. This finding aligns with those of Curtright and Turner [ 13] and Cohen-Mansfield [ 14]. Our results also suggest that tactile stimuli should be implemented for more success, based on the findings that 3 of the 4 residents had the most vocalizations during physical games, which accords with results of studies that found tangible stimuli to elicit more meaning-enriched statements, perhaps due to the shared context created by the stimuli [ 11, 13]. Use of trivia-fill-in activities are not recommended, suggested based on the lack of vocalizations during these activities, and the qualitative notes that residents appeared bored. If used, adding a tactile element to trivia/fill-ins might assist with engagement (e.g. tossing a ball to establish turns to answer, or using trivia based on a stimulus).
Facilitators
Throughout the collection period, most sessions were led by an intern and a volunteer. Little information about the training of these individuals was available; however, all of them were gerontology students at a nearby university, so they had relevant college coursework regarding aging. Most of the students seemed to have little experience working with PWDs and/or leading activities. Given the importance of the facilitator in structuring activities to be optimal for all participants, training for novice activities leaders has the potential to enhance the success of activities programs.
Communication dominators
Communication domination can occur in any group setting, but it is particularly relevant in groups with varying language abilities, such as group activities with PWDs, or group aphasia therapy. Facilitators in group therapy address an important concern: if one participant dominates the floor, participants with less language ability lose opportunities to participate [ 25]. This concern is also present for groups of PWDs, and should be addressed because communication allows PWDs both to form relationships [ 7], and to construct selves [ 4, 6]. Although it is premature to make definitive suggestions, a few possible ideas to better facilitate activities arose from the data. First, turn taking structures and tangible stimuli could be used in activities. Next, strategies to deal with groups with varying language levels, perhaps similar the following which are based on aphasia therapy, could also be taught to staff:
Prompting and encouraging residents to engage in the discussion; [25] Using strategies to ensure equal participation, including encouraging more vocal participants to be patient with others [24], and employing strategies such as structured turn-taking to allow for all to participate; [25] Using strategies such as yes-no questions, even rates of speech, and simplified sentences to better communicate with PWDs (see Small [9,] and Small and Perry [10] for reviews); Taking on an initiating role by generating more opening statements; [22] Accompanying verbal cues with gestures and postural cues when facilitating all types of activities [23].
Limitations
This study had several limitations, many of which were related to feasibility concerns of live data coding. A larger sample size and more complex coding scheme were not feasible, due to the finite ability of human coders in the moment. This limited the level of detail and richness of data available (e.g., nonverbal communication, and exact transcription of utterances). As a small-scale qualitative investigation, the results are suggestive but in need of confirmation using methods with generalizability.
Reliability
Although reliability overall was high, three categories received lower scores, thus any conclusions based on these categories are tentative. The lower scoring items generally had fewer exemplars than other categories, so coders had fewer opportunities to practice on them and thus refine the coding manual accordingly.
The difference between the reliability scores of the individual vocalization categories and total vocalizations shows that, while coders usually agreed that a vocalization was made, the categorization was a challenge. This concern could be addressed by use of a longer training period, and/or by using video data allowing coders to re-watch and discuss coding inconsistencies. Despite these concerns, the principal investigator achieved best reliability with the more advanced coder, thus supporting the robustness of the coding schema and bolstering confidence in the replicability of the codes.
Summary
This study found that the activity that elicited the most vocal communication for the most participants was physical games, while trivia/fill-in elicited the least vocalizations. Individual differences were observed: one participant showed the opposite pattern. Potential reasons for these differences include variations in the activity, facilitators, and participants. More research is needed on how to maximize communication during activities for PWDs, including use of video for data collection, and studies using experimental designs exploring such interventions as staff training. Nonetheless, the present preliminary findings suggest the potential for facilitation techniques that take into account individual differences, coupled with careful selection of activities, to enhance success in preserving cognitive and communicative function among persons with dementia. Appropriate and socially engaging daily activities can enhance the quality of life for this vulnerable and under-served population.
Figure 1
Vocalization type by activity: Participant 1. 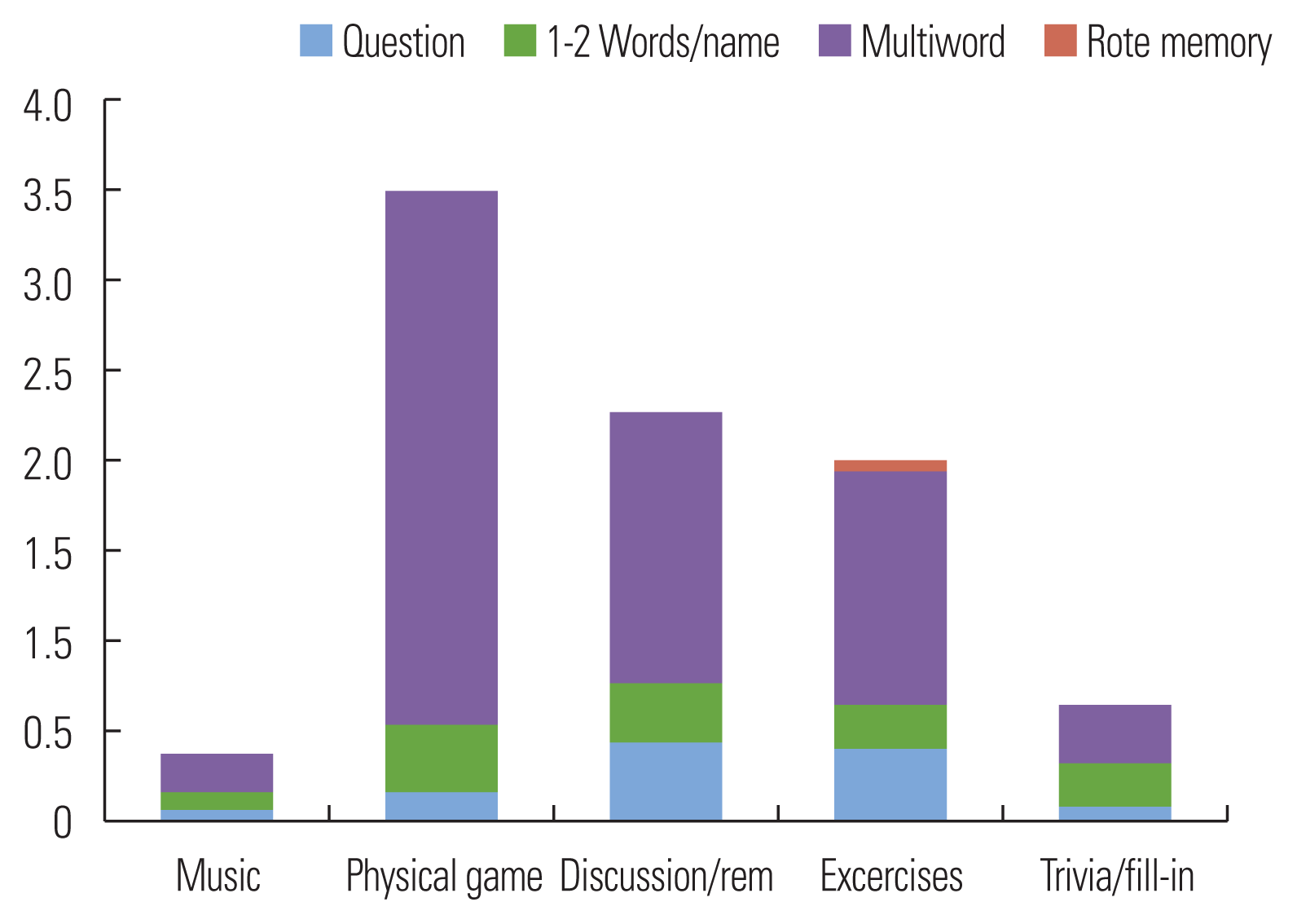
Figure 2
Vocalization type by activity: Participation 2. 
Figure 3
Vocalization types by activity: Participant 4. 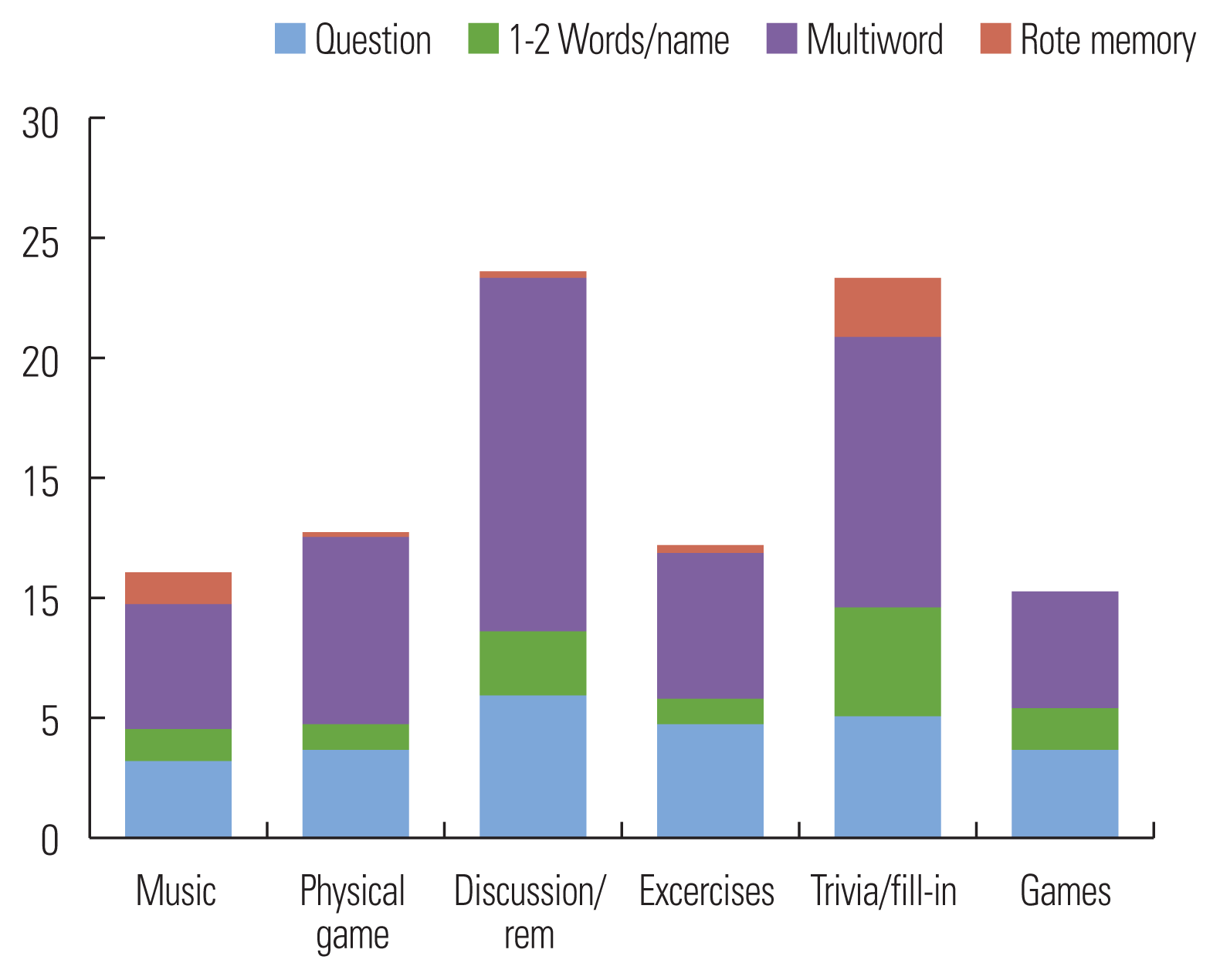
Figure 4
Types of vocalizations by activity: Participant 5. 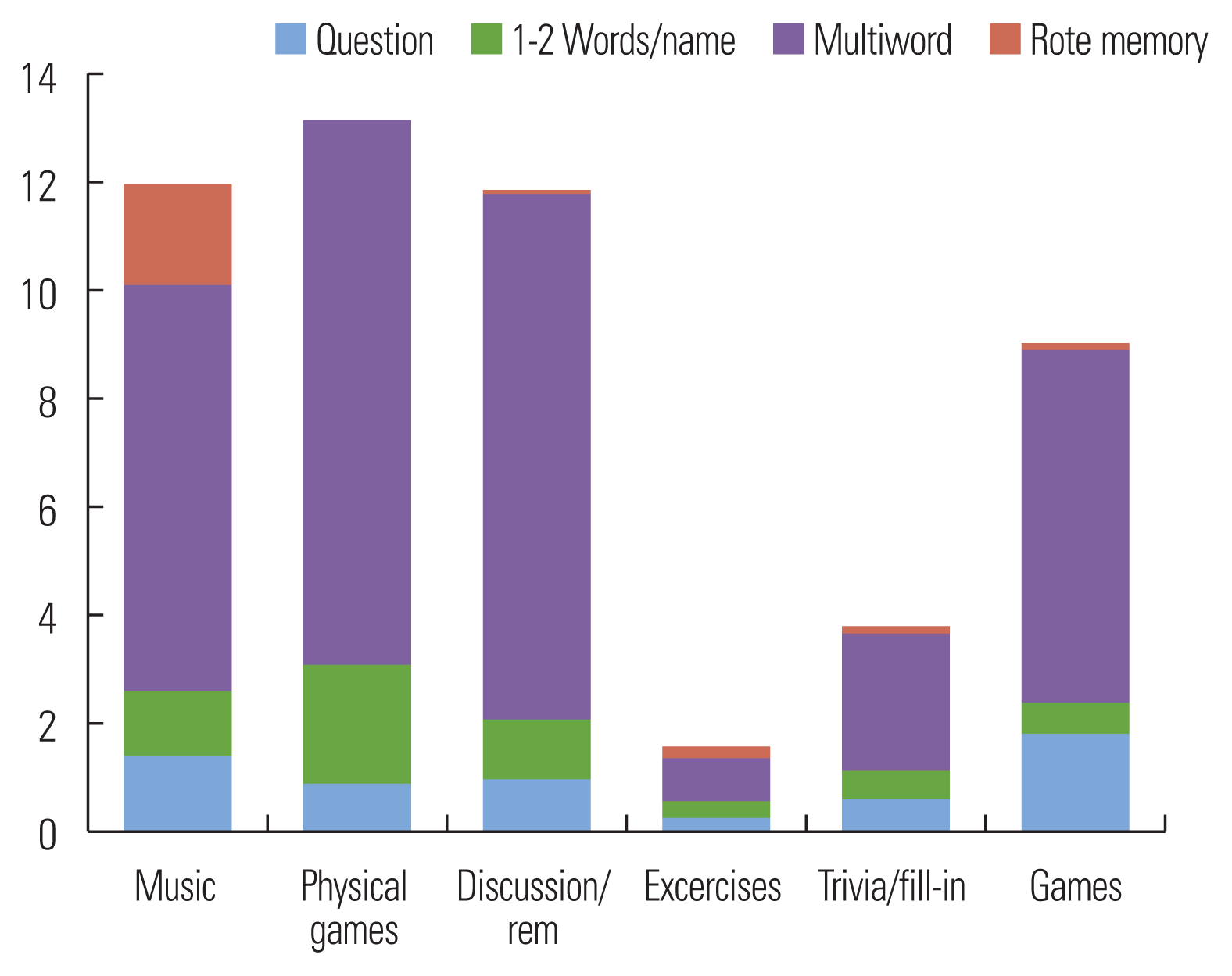
Table 1
Vocalization type by activities: P1
|
Activity |
Question |
Command |
1–2 Words/name |
Multiword |
Rote memory |
Nonword |
Total acts |
|
Music |
0.08 |
0.00 |
0.08 |
0.23 |
0.00 |
0.61 |
1.36 |
|
Physical game |
0.15 |
0.02 |
0.40 |
2.95 |
0.00 |
0.74 |
4.90 |
|
Discussion/rem |
0.43 |
0.05 |
0.33 |
1.52 |
0.00 |
0.43 |
3.59 |
|
Exercises |
0.39 |
0.00 |
0.26 |
1.30 |
0.06 |
1.04 |
3.38 |
|
Trivia/fill-in |
0.07 |
0.00 |
0.24 |
0.34 |
0.00 |
0.22 |
1.16 |
Table 2
Vocalization type by activities: P2
|
Activity |
Question |
Command |
1–2 Words/name |
Multiword |
Rote memory |
Nonword |
Total acts |
|
Music |
0.61 |
0.00 |
0.74 |
1.82 |
0.00 |
0.27 |
4.19 |
|
Physical game |
0.40 |
0.03 |
0.47 |
2.45 |
0.00 |
0.06 |
4.60 |
|
Discussion/rem |
0.00 |
0.00 |
0.00 |
0.23 |
0.00 |
0.00 |
0.30 |
|
Exercises |
0.05 |
0.29 |
0.24 |
0.97 |
0.00 |
0.05 |
1.84 |
|
Trivia/fill-in |
0.16 |
0.02 |
0.23 |
0.44 |
0.05 |
0.00 |
0.96 |
Table 3
Vocalization types by activity: P4
|
Activity |
Question |
Command |
1–2 Words/name |
Multiword |
Rote memory |
Nonword |
Total acts |
|
Music |
3.44 |
0.25 |
1.19 |
5.35 |
1.21 |
0.02 |
11.58 |
|
Physical game |
3.73 |
0.38 |
1.20 |
7.76 |
0.09 |
0.26 |
13.82 |
|
Discussion/rem |
6.06 |
0.29 |
2.65 |
15.03 |
0.11 |
0.32 |
24.74 |
|
Exercises |
4.78 |
0.31 |
1.21 |
6.21 |
0.09 |
0.13 |
12.86 |
|
Trivia/fill-in |
5.25 |
0.27 |
4.48 |
11.40 |
2.26 |
0.40 |
19.16 |
|
Games |
3.84 |
0.12 |
1.62 |
4.88 |
0.00 |
0.03 |
6.83 |
Table 4
Vocalization types by activity: P5
|
Activity |
Question |
Command |
1-2 Words/name |
Multiword |
Rote memory |
Nonword |
Total acts |
|
Music |
1.34 |
0.18 |
1.26 |
7.57 |
1.83 |
1.28 |
13.51 |
|
Physical game |
0.92 |
0.92 |
2.18 |
10.03 |
0.00 |
0.60 |
15.40 |
|
Discussion/rem |
1.01 |
0.02 |
1.05 |
9.68 |
0.06 |
0.41 |
12.58 |
|
Exercises |
0.30 |
0.00 |
0.25 |
0.85 |
0.20 |
0.30 |
2.00 |
|
Trivia/fill-in |
0.63 |
0.00 |
0.45 |
2.58 |
0.14 |
0.07 |
4.03 |
|
Games |
1.74 |
0.03 |
0.64 |
6.62 |
0.06 |
0.27 |
9.60 |
REFERENCES
2. Byrne K, Orange JB. Conceptualizing communication enhancement in dementia for family caregivers using the WHO-ICF framework [Internet]. Advances in Speech Language Pathology. 2005. [cited 2017 May 8]. 7(4):187–202. http://dx.doi.org/10.1080/14417040500337062.  4. Roland Kaitlyn P, Chappell Neena L. Meaningful activity for persons with Dementia family caregiver perspectives [Internet]. American Journal of Alzheimer’s Disease and Other Dementias. 2015. [cited 2017 May 8]. https://doi.org/10.1177/1533317515576389.  5. Leedahl SN, Chapin RK, Little TD. Multilevel examination of facility characteristics, social integration, and health for older adults living in nursing homes [Internet]. The Journals of Gerontology Series B: Psychological Sciences and Social Sciences. 2014. [cited 2017 May8]. 70(1):111–122. https://doi.org/10.1093/geronb/gbu112.   7. Müller N, Mok Z. Applying systemic functional linguistics to conversations with dementia: The linguistic construction of relationships between participants. Seminars in Speech and Language. 2012. [cited 2017 May 8]. 33(01):5–15. https://doi.org/10.1177/1471301213488609.    9. Small JA, Gutman G, Makela S, Hillhouse B. Effectiveness of communication strategies used by caregivers of persons with Alzheimer’s disease during activities of daily living [Internet]. Journal of Speech, Language, and Hearing Research. 2003. [cited 2017 May 8]. 46(2):353–367. http://sig15perspectives.pubs.asha.org/article.aspx?articleid=1781185.  12. Smit D, de Lange J, Willemse B, Twisk J, Pot AM. Activity involvement and quality of life of people at different stages of dementia in long term care facilities [Internet]. Aging and Mental Health. 2016. [cited 2017 May 8]. 20(1):100–109. http://dx.doi.org/10.1080/13607863.2015.1049116.   13. Curtright A, Turner GS. The influence of a stuffed and live animal on communication in a female with Alzheimer’s dementia. Journal of Medical Speech-Language Pathology. 2002;[cited 2017 May 8]. 10(1):61–72.
14. Cohen-Mansfield J, Thein K, Dakheel-Ali M, Regier NG, Marx MS. The value of social attributes of stimuli for promoting engagement in persons with dementia [Internet]. The Journal of Nervous and Mental Disease. 2010. [cited 2017 May 8]. 198(8):586–596. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3139232/.    16. Cabrera E, Sutcliffe C, Verbeek H, Saks K, Soto-Martin M, Meyer G. Non-pharmacological interventions as a best practice strategy in people with dementia living in nursing homes: A systematic review [Internet]. European Geriatric Medicine. 2015. [cited May 8]. 6(2):134–150. https://doi.org/10.1016/j.eurger.2014.06.003.  19. Douglas NF, McDonald K. Interprofessional Care in the Management of Alzheimer’s Dementia: Leaving Our Silos. Perspectives of the ASHA Special Interest Groups SIG 2. 2016;[2017 May 8]. 1(2):129–137.  20. Halliday M, Mathiessen C. An introduction to functional grammar. 2004. [cited 2017, May 8]. p. 3New York, NY: Oxford University Press Inc.
21. Sung HC, Chang AM, Lee WL. (2010). A preferred music listening intervention to reduce anxiety in older adults with dementia in nursing homes. Journal of Clinical Nursing. 2018;[cited 2017 Oct 13]. 19(7–8):1056–1064.  22. Eggins S. An Introduction to Systemic Functional Linguistics. Continuum International Publishing Group, New York: 2004. [cited 2017 May 8].
24. Bernstein-Ellis E. Aphasia group communication treatment: The aphasia center of California approach. Group treatment of neurogenic Communication disorders: The expert clinician’s approach. 2006;[cited 2017 May 8]. 2:71–75.
25. Archer B. (2016). Facilitated group conversations for people with aphasia: A cognitive ethnographic study. University of Louisiana, Lafayette: Doctoral dissertation. 2016. [cited 2017 May 8]. 9781369180138.
Appendices
Appendix A
Coding Manual for Data Collection
Demanding
This term is another word for requesting. This category is broken down into a question or command.
Giving
This term means they are responding to or spontaneously beginning new discourse. This category is broken into either a statement or an offer.
-
Statement: provides information, as either an answer to a question, or in a spontaneous utterance.
- 1–2 words/a name (“yes, please” or “Billy Ray Cyrus”) or - multiword utterance (“I am good”),
-
Offer: contributes a good or service as either an answer to a question or in a spontaneous utterance. This could also include a question: “would you like me to…?”
General
These are communicative behaviors that do not necessarily further or begin a conversation, including exclamations, pieces of rote memory, vocalizations, or meaningful gestures.
-
Exclamations: stereotypical words or phrases that are often said in response to events to express shock, enjoyment, or even displeasure.
-
Rote memory: multi-word utterances that are known by heart by the individual
-
- Examples: Songs, Nursery Rhymes, Counting, Naming months, days, colors prayers
*** This DOES INCLUDE FILL IN THE BLANK “SAYINGS”
-
- example:
- prompt: “an apple a day____” - finishing phrase: “keeps the doctor away” - Prompt: “Yankee doodle___” -finishing phrase: “Dandy”
-
Nonverbals:
-
Nonword vocalization: a vocalization that cannot be discerned as a word, but is a result of the activity, or something said by another person.
-
Meaningful Gesture: a gesture meant to convey a - meaning.
Engagement: former can be rated from one to seven, one being not at all engaged at any point, and 7 being highly engaged throughout Affect: can be rated as negative, flat or positive
|
|